Overview
Crohn’s disease is a chronic inflammation that may occur anywhere along the gastrointestinal tract. It’s most commonly found in the distal ileum. It can be painful and debilitating
The exact cause of Crohn’s disease is unknown, but it is possible that it is related to abnormal gut bacterium. A genetic component may be also be implicated as Crohn’s is more common in people with a familial history of Crohn’s (Lewis, 2016).
Here’s a short introductory video:
Signs & Symptoms
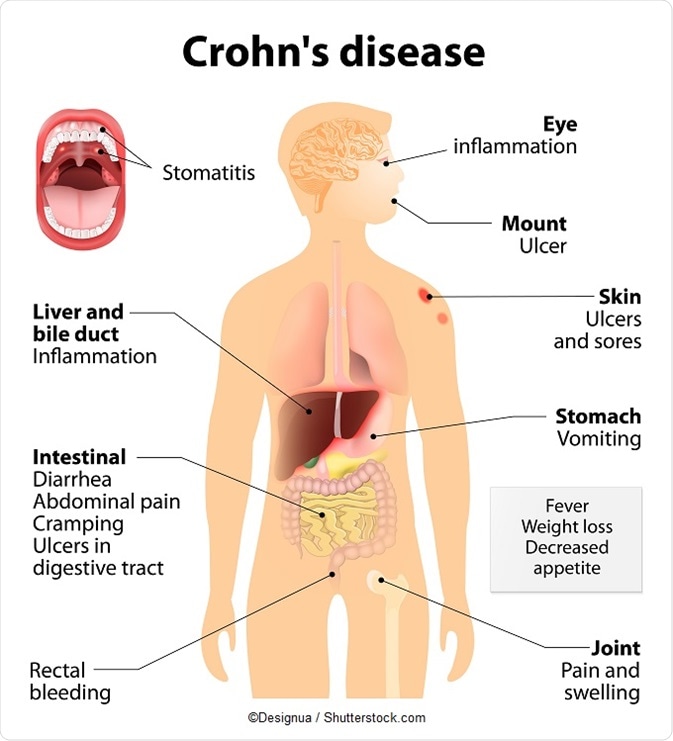
- Signs and symptoms of Crohn’s disease may include:
- Diarrhea
- Fever
- Abdominal pain and cramping
- Blood in the stool
- Mouth sores
- Reduced appetite and weight loss
- Pain or drainage near or around the anus due to inflammation from a fistula
Diagnostic Tests
- Blood tests for anemia or infection
- Fecal occult blood test (hidden blood in the stool)
- Colonoscopy and Computerized tomography for visualization of the gastrointestinal tract
Treatment
Treatment for Crohn’s disease focuses on the symptom management of reducing inflammation. Pharmacological treatments can include anti-inflammatories (corticosteroids, oral 5-aminosalicylates), immunosuppressants (Azathioprine, Methotrexate), antibiotics (Cipro, Flagyl), anti-diarrheals (Metamucil, Citrucel), pain relievers (Tylenol), Iron supplements, vitamin B-12 injections, and calcium and vitamin D supplements (Lewis, 2016).
Diet
Keeping a food diary may help to identify foods are tolerable and which cause exacerbation
In addition, people with Crohn’s may want to:
- Limit dairy products
- Try low-fat foods
- Limit fiber during exacerbations
- Eat small meals
- Drink plenty of fluids
Flare-ups
Occasional flare-ups can happen with Crohn’s disease. Below is a video from the Crohns & Colitis Foundation with advice concerning diet during flare-ups.
