Ulcerative Colitis is an ulcerative and inflammatory disease of the bowel that results in poor absorption of nutrients. This disorder usually begins at the rectum and spreads upward towards the colon. The incidence of ulcerative colitis is highest in Caucasians and people of Jewish heritage (Smeltzer & Bare, 2004). The peak incidence is between ages 30 and 50 years of age.
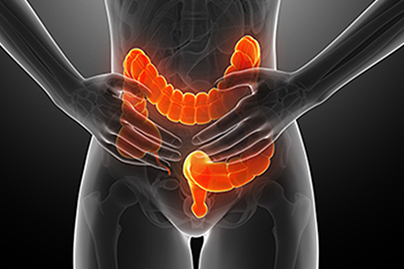
The colon becomes edematous and may develop lesions and ulcer.
Colitis is characterized by various periods of remissions and exacerbations and can be classified as mild, severe or fulminant (severe and sudden).
SIGNS & SYMPTOMS
Abdominal cramping, bloody diarrhea (10 to 20 liquid stools/day), tenesmus (urgent defecation), fever, vomiting, weight loss, malaise, decreased iron absorption, malnutrition & dehydration
TESTS
Barium enema, sigmoidoscopy.
TREATMENTS
Antibiotics eg. Flagyl are used for secondary infections such as peritonitis and abscesses.
Antidiarrheals- used to minimize peristalsis, until stools approach normal consistency and frequency
Aminosalicylates- eg. Sulfasalazine used to prevent or reduce recurrence.
Steroids- eg.Prednisone in severe or fulminant cases.
Immunomodulators- eg. Imuran have been used to alter the immune response (Wolf,2000).
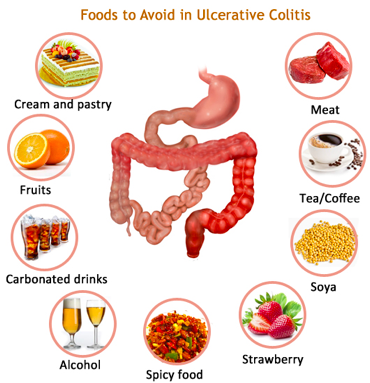
FOODS TO AVOID
Any foods that exacerbate diarrhea should be avoided. Milk, cold foods and smoking are avoided because they increase intestinal motility.

FOODS ALLOWED
Oral fluids, low fiber diet during exacerbation. High protein with vitamins
and iron supplements.
Complications of Ulcerative Colitis
Some complications are toxic mega colon which is associated with a high mortality rate (15% to 50%) (Smeltzer et al., 2004). Eventually, 15% of patients may develop carcinoma of the colon.
